Scar revision encompasses a range of techniques designed to improve the appearance and functionality of scars. While no method can entirely erase a scar, procedures can minimize its visibility, reduce discomfort, and restore lost tissue function. This article provides a comprehensive overview of available treatments, potential risks, and what patients should expect during the process.
Understanding Scars and Why Revision Matters
Scars form as the natural result of skin injury – whether from surgery, burns, trauma, or conditions like acne. The body replaces healthy tissue with fibrous collagen, creating a visible mark. While some scars fade over time, others remain prominent, causing cosmetic concerns or functional limitations. Scar revision isn’t just about aesthetics; it can address pain, restricted movement, and psychological distress.
Treatment Options: From Topical Care to Surgery
The best approach depends on the scar’s type (keloid, hypertrophic, atrophic, contracture), severity, location, and the patient’s goals. Treatments fall into several categories:
Topical Therapies: Best suited for new or mild scars, these include pressure dressings, polyurethane sheets, and silicone gels. These reduce inflammation and encourage flatter, less noticeable scars. Consistency is key; daily application for months may be required.
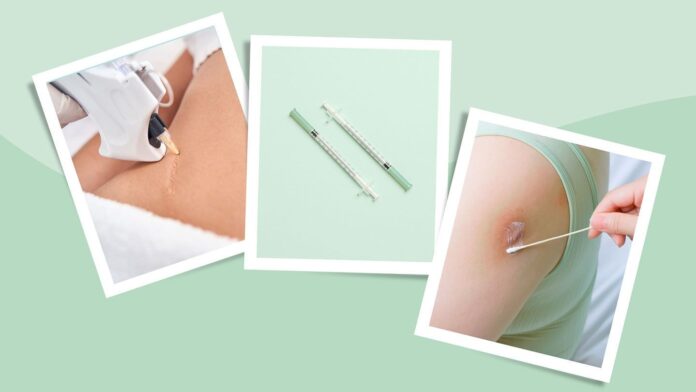
Injectables: For raised scars (keloids and hypertrophic scars), injections of corticosteroids or chemotherapy drugs (5-FU, bleomycin) can shrink the tissue and relieve discomfort. Dermal fillers are used for indented scars (acne scars), temporarily restoring volume.
Skin Resurfacing: These methods smooth irregularities and reduce pigmentation. Options include laser therapy (effective for all scar types), cryotherapy (freezing the scar), chemical peels, and dermabrasion (mechanical smoothing). Microneedling stimulates collagen production for improved texture.
Surgical Techniques: For severe or large scars, surgery may be necessary. Z-plasty and W-plasty reshape the scar to align with natural skin tension, improving movement. Skin grafts replace missing tissue (common in burn scars), while direct excision removes the scar entirely.
Who Is a Good Candidate?
Ideal candidates are physically healthy, have realistic expectations, and don’t smoke. Patients with underlying skin conditions in the treatment area or who are unwilling to commit to long-term care may not see optimal results. Scar revision works best when patients understand that scars can be improved, not eliminated.
Preparing for the Procedure
Before treatment, a healthcare provider will assess the scar and rule out malignancy. Anesthesia options range from local numbing to full sedation, depending on the procedure’s complexity. Patients should disclose all medications, allergies, and medical conditions. Doctors may recommend vitamin-rich diets and avoiding smoking to optimize healing.
Recovery and Potential Risks
Recovery varies by technique but typically involves weeks to months of healing. Stitches may be removed after a few days, and normal activities can often be resumed shortly after. However, patients should avoid stretching the new scar and protect it from sun exposure.
Potential risks include discomfort, swelling, discoloration, infection, and (rarely) further scarring. Serious complications like shortness of breath or fever warrant immediate medical attention.
The Bottom Line
Scar revision offers viable solutions for improving the appearance and function of scars. The appropriate treatment depends on individual factors, and realistic expectations are crucial. While risks exist, modern techniques can significantly reduce scar visibility and improve quality of life.